The Complete Guide to Minimally Invasive Hip Replacement Surgery: Smaller Incision, Rehab-Free Recovery, Regain Your Stride
【Article Summary】 If you find yourself experiencing a dull pain in your hip when walking, unable to squat, or even struggling to put on shoes and socks, this may be a signal from your hip joint. In the past, the term "joint replacement" often evoked fear of large incisions and dislocation. However, modern "minimally invasive" techniques allow the joint replacement to be performed through natural muscle planes, without cutting the muscles, with significantly improved precision. Many patients can even "walk on the same day after surgery." This article will provide you with an in-depth understanding of minimally invasive total hip replacement surgery.
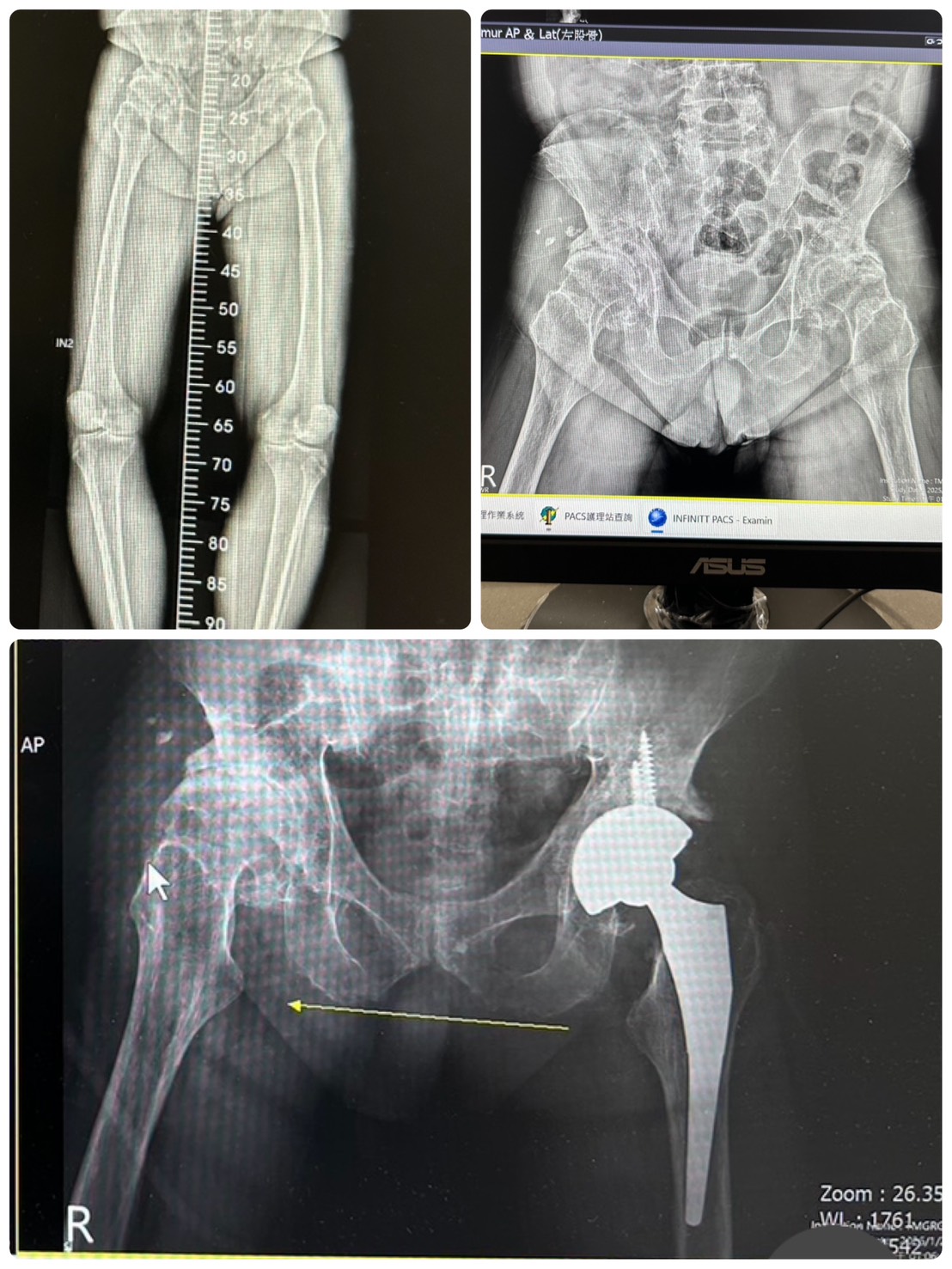
The Root of Hip Pain: When Should You Consider Replacement Surgery?
The hip joint is the body's largest weight-bearing ball-and-socket joint, composed of the femoral head and the acetabulum. When the protective cartilage wears down to the point of "bone-on-bone" contact, it leads to the following conditions that impact daily life:
Common Indications
-
Osteoarthritis of the Hip: Long-term wear and tear leading to the loss of joint space.
-
Avascular Necrosis of the Femoral Head: Often associated with alcohol abuse or long-term steroid use, causing collapse of the bone tissue.
-
Rheumatoid Arthritis: The body's autoimmune system attacks the joint's synovial membrane.
-
Post-Traumatic Arthritis: A sequela following fractures or severe dislocations.
When to Transition from "Conservative Treatment" to "Surgical Evaluation"?
So, when should one consider hip replacement surgery? Dr. Chien-Chun Chang's team recommends seeking a professional evaluation if the following situations apply:
-
Medications Are Ineffective: Non-steroidal anti-inflammatory drugs (NSAIDs) can no longer alleviate the pain.
-
Significant Functional Limitations: Inability to climb stairs comfortably, or even experiencing pain at rest.
-
Substantial Decline in Quality of Life: Pain leads to social withdrawal or chronic insomnia.
In-Depth Comparison of Surgical Approaches: Traditional vs. Minimally Invasive
The difference between "traditional" hip replacement surgery and "minimally invasive" hip replacement surgery lies in the fact that the core of the minimally invasive approach is "tissue preservation," which also aims to reduce the skin incision, making the patient's recovery process easier. Based on the path of entry into the joint, it is primarily divided into the following three main paradigms:
Traditional Posterior Approach
This is the oldest and offers the clearest surgical field of view.
-
Technical Limitation: Requires cutting part of the gluteus maximus muscle and severing the external rotator muscles.
-
Disadvantage: Because the posterior "joint capsule" support is disrupted, there is a higher risk of dislocation in the early postoperative period (approximately 1-3%), and the rehabilitation period is longer.
Anterolateral Approach
This is considered an option between the Direct Anterior Approach and the Posterior Approach.
-
Technical Characteristic: The incision is made on the outer side of the thigh, involving the gluteus medius muscle (a key muscle for maintaining walking balance).
-
Advantage: Postoperative dislocation rate is lower than the posterior approach.
-
Disadvantage: If the gluteus medius muscle is significantly damaged during surgery, a temporary "Trendelenburg gait" (a waddling walk) may occur postoperatively.
Direct Anterior Approach (DAA)
Currently the internationally recognized minimally invasive approach with the fastest recovery.
-
Technical Advantage: Utilizes a natural intermuscular plane (between the tensor fasciae latae and sartorius muscles) to access the joint without cutting any muscles.
-
Advantage: Patients can bear weight and walk on the same day after surgery. Because the posterior tissues remain intact, there are virtually no posture restrictions postoperatively (no need for anti-dislocation pillows or extreme precautions).
Innovative Anterolateral Minimally Invasive Hip Replacement Surgery
Dr. Chien-Chun Chang's innovative minimally invasive technique promotes rapid recovery with minimal need for formal rehabilitation.
-
Technical Advantage: An anterolateral incision is used to completely preserve the hip joint capsule and surrounding musculature. The joint replacement is performed without cutting any muscles, significantly reducing tissue trauma.
-
Advantage: Due to the complete preservation of the joint capsule and muscle structure, patients experience significantly reduced postoperative pain and accelerated recovery. Typically, patients can be discharged within 2-3 days after surgery, and the duration of walker use is greatly shortened. As formal rehabilitation is often not required, most patients can wean off walking aids earlier and quickly return to daily activities and normal life.
The Core of Surgical Choice is "How to Help You Return to Life with Ease"
If you, like most patients, hope that "after surgery, there are as few complications as possible and a return to normal life as quickly as possible," then the key to choice lies in "how little disruption the surgery causes to the body." Traditional surgery is like building a major road—stable but involving a large-scale project, resulting in slower recovery and more restrictions. The goal of minimally invasive surgery is to reduce this "construction" disruption. Among these techniques, the "anterior" or "anterolateral" approaches, because they do not cut important muscles, have become the choice that allows patients a more comfortable recovery.
-
Lighter Pain: Because tissue disruption is minimized.
-
Rapid Recovery: Hospital stay of 2-3 days, and soon no longer needing a walker.
-
No Need for Extensive Rehab Commutes: With the body's structure largely preserved, natural movement itself becomes the best form of recovery.
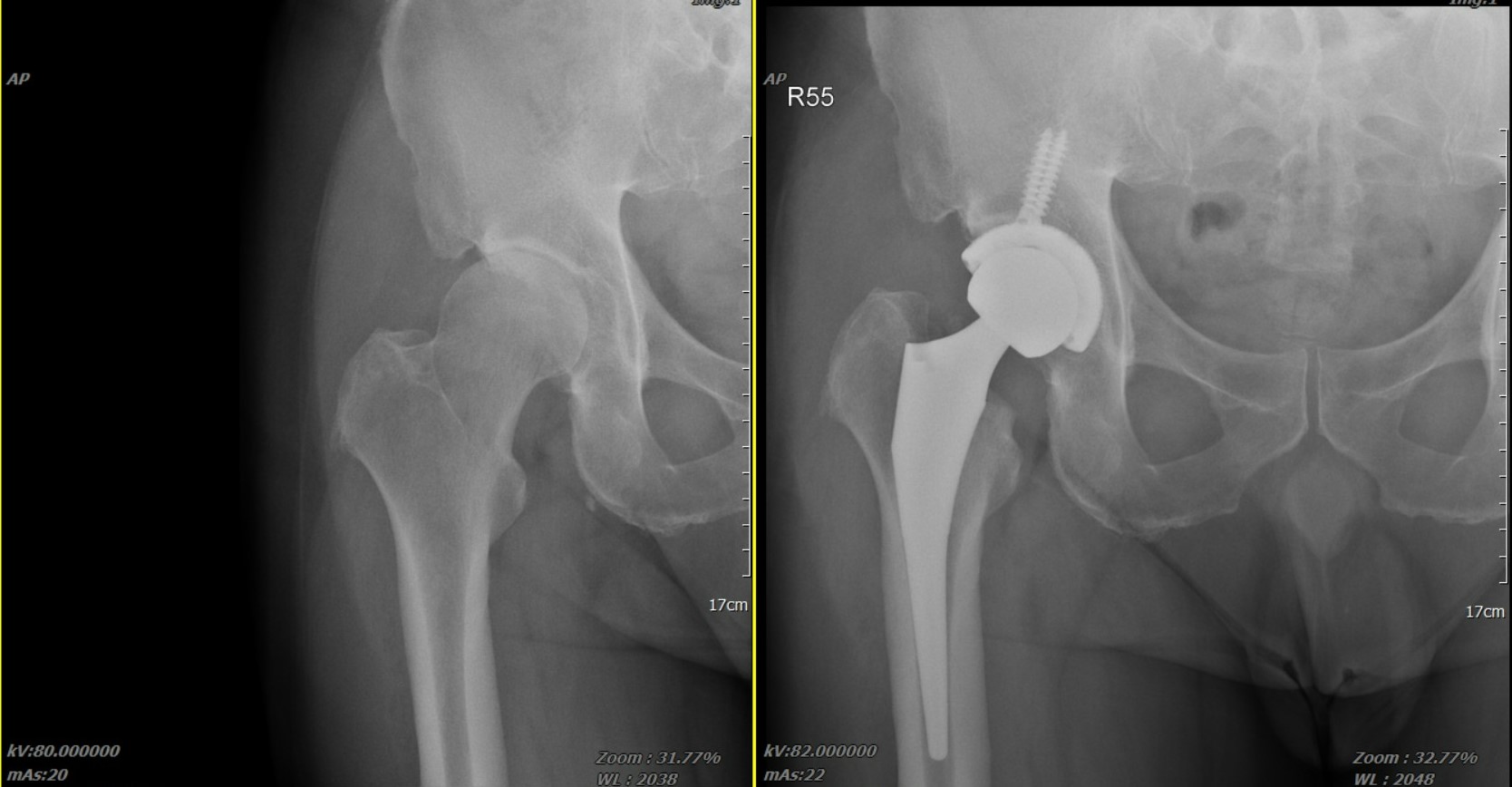
In summary, the goal of this innovative technology is to minimize the impact of surgery on your life. It transforms joint replacement from a "major ordeal" requiring a long-term battle into a "stage of treatment" that can be resolved quickly. It is recommended that you bring these comparisons to discuss with your attending physician. Together, based on your specific situation, you can choose the surgical approach that is most suitable for you and allows you to return to life with the least burden.
Perspective of Evidence-Based Medicine: Clinical Outcomes of Minimally Invasive Surgery
Dr. Chang provides references to medical journal literature and clinical data (as reported in publications such as BMC Musculoskeletal Disorders) for your consideration:
| Indicator | Traditional Surgery | New Minimally Invasive Surgery | Clinical Significance |
| Average Blood Loss | 500-800 ml | 100-200 ml | Reduces transfusion risk and cardiopulmonary stress. |
| Hospital Stay | 7-10 days | 2-5 days | Decreases risk of bedrest complications and lowers healthcare costs. |
| Pain Index (VAS) | Higher | Significantly Lower | Enables earlier initiation of functional rehabilitation after surgery. |
| Dislocation Risk | 2-4% | <1% | Postoperative posture restrictions (e.g., squatting, crossing legs) are significantly reduced. |
Material Selection: Analysis from NHI-Covered to Out-of-Pocket Options
Comparison of Artificial Hip Replacement Materials
| Artificial Acetabular Cup | Liner | Artificial Femoral Head | Surgical Cost | Features |
Acetabular Cup |
Polyethylene | Ceramic | NT$60,000 | Wear-resistant |
| Vitamin E-Infused Polyethylene | NT$180,000 | Wear-resistant, Impact-resistant | ||
| 3D-Printed Acetabular Cup | Vitamin E-Infused Polyethylene | Ceramic | NT$240,000 |
Wear-resistant, Impact-resistant, 80% faster wound healing, can squat
|
|
Dual-Mobility Acetabular Cup
|
Vitamin E-Infused Polyethylene | Ceramic | NT$280,000 |
Wear-resistant, Impact-resistant, faster wound healing, can squat
|
Evidence-Based Medical Data: Postoperative Functional Assessment
Postoperative Recovery Progression Chart
| 時間點 | 康復目標 | 物理治療重點 |
| 術後 0-6 小時 | 意識恢復、床上翻身 | 多模式止痛管理、踝泵運動 |
| 術後 24 小時 | 輔具站立與行走 | 踏步練習、轉位訓練 |
| 術後 2 週 | 傷口癒合、居家步行 | 臀中肌強化、核心穩定練習 |
| 術後 6 週 | 脫離單拐、恢復日常生活 | 步態修正、耐力訓練 |
| 術後 3 個月 | 恢復運動(如游泳、高球) | 本體感覺訓練、多向活動度優化 |
Complication Management and Risk Prevention
Although minimally invasive surgery is very safe, we still approach the rare risks with a rigorous medical attitude:
-
Thrombosis Prevention (DVT): It is recommended to get out of bed on the day of surgery. Preoperative education includes teaching ankle pump exercises, which should be continued postoperatively.
-
Wound Care: We utilize watertight subcuticular cosmetic sutures, which significantly reduce the pathway for bacterial invasion.
-
Periprosthetic Fracture: Through the precise force control of robotic-arm assistance during implantation, the risk of intraoperative bone fracture can be avoided.
FAQs on Minimally Invasive Hip Replacement Surgery
Q: Should I wait until the pain is unbearable and I can't walk before having surgery?
Physician's Answer: It is not recommended. Long-term endurance of pain can lead to "disuse muscle atrophy" and spinal compensation. Once muscles atrophy, the postoperative rehabilitation period doubles. It is advisable to seek evaluation before the cartilage is completely worn away.
Q: Is minimally invasive surgery effective for overweight (obese) individuals?
Physician's Answer: Minimally invasive hip replacement is more challenging for obese patients, but an experienced team can complete it using specialized instruments. In fact, obese patients benefit more from minimally invasive techniques to lower the risk of wound infection.
Q: How do I choose the material for the artificial joint? Metal or ceramic?
Physician's Answer: Ceramic is currently the mainstream choice, offering the highest wear resistance and excellent biocompatibility. Metal components may be suitable for older individuals with lower activity levels.
Q: How long after surgery can I drive?
Physician's Answer: For right leg surgery, typically 4-6 weeks are needed for reaction time to recover. For left leg surgery with an automatic transmission car, driving may be attempted sooner after surgery.
Q: Will the surgery cause "leg length discrepancy"?
Physician's Answer: This was indeed a risk with traditional surgery. However, minimally invasive surgery, combined with surgeon skill and technique, can minimize this difference. Sometimes, to ensure optimal joint tension based on the patient's specific condition, minor adjustments may still be necessary.
Q: I have heart disease/diabetes. Can I still have the surgery?
Physician's Answer: Yes, if preoperative HbA1c is controlled below 7.0 and a cardiologist assesses stable blood flow, surgery can be considered. Due to its minimal physiological disturbance, minimally invasive surgery is actually a safer option for high-risk patients.
Q: Can I squat or use a squat toilet after surgery?
Physician's Answer: Patients undergoing minimally invasive hip replacement can begin assisted deep squats 2 weeks post-surgery once the wound is stable, with minimal impact on daily function. With the latest dual-mobility hip implants, most patients can achieve a squatting position postoperatively.
Q: Will the artificial joint need to be replaced in a second surgery (revision)?
Physician's Answer: With modern, highly wear-resistant materials, most artificial joints can last at least 20-30 years, potentially even over 40 years. For ceramic-on-ceramic pairings, the lifespan can be 30-40 years. Unless complications like infection or loosening due to severe osteoporosis occur, most people only need this surgery once in their lifetime.
Dr. Chien-Chun Chang's Concluding Thoughts: Choose Precision, Choose Freedom
The evolution of minimally invasive hip replacement surgery marks medicine's transition from "traditional disruption" to "minimally invasive preservation." This is more than just a surgical procedure; it is an opportunity to reclaim the freedom of your life. When technology can reduce surgical error to under 1 cm, you no longer need to fear a large incision or compromise your life due to persistent pain.
Disclaimer: This article is for educational purposes only. Please consult a qualified physician for specific medical advice.






