The Complete Guide to Minimally Invasive Cervical Spine Surgery: How "Navigated Minimally Invasive" Techniques Precisely Relieve Nerve Compression and Speed Recovery
Numb hands, weakness, unsteady gait—when cervical nerves are compressed, your quality of life suffers. Do you feel anxious upon hearing that cervical spine surgery might be needed, fearing the large incision, long rehabilitation, and complications of traditional surgery?Today, cervical spine surgery has entered the era of "precision minimally invasive" techniques. The Dr. Chien-Chun Chang Minimally Invasive Spine & Joint Team, with the assistance of "3D computer navigation" and "high-end endoscopy", can select the least traumatic approach based on your specific type and location of compression to achieve the goal of effective decompression and rapid recovery.
Anterior Cervical Surgery (Anterior Approach)
Anterior cervical surgery is commonly used for central or paracentral disc herniations, anterior vertebral bone spurs, spinal canal stenosis, and other pathologies. The procedure involves a small incision of about 1-2 cm in the front of the neck. After gently retracting the trachea, esophagus, and carotid artery through natural tissue planes, the disc material compressing the spinal cord or nerves is removed under endoscopic guidance. If necessary, an interbody cage or artificial disc is implanted to restore disc height and stability.
Advantages & Risks of Anterior Cervical Surgery
Advantages:
-
Stable Decompression: Fusion provides excellent long-term stability.
-
Preserved Mobility (with Artificial Disc): Artificial disc replacement can maintain motion at that level.
Risks & Considerations:
-
Recovery Period: Hospital stay is typically 1-3 days, with full recovery taking several weeks to months.
-
Potential Complications: May include temporary swallowing difficulties, adjacent segment degeneration, or pseudoarthrosis (non-fusion).
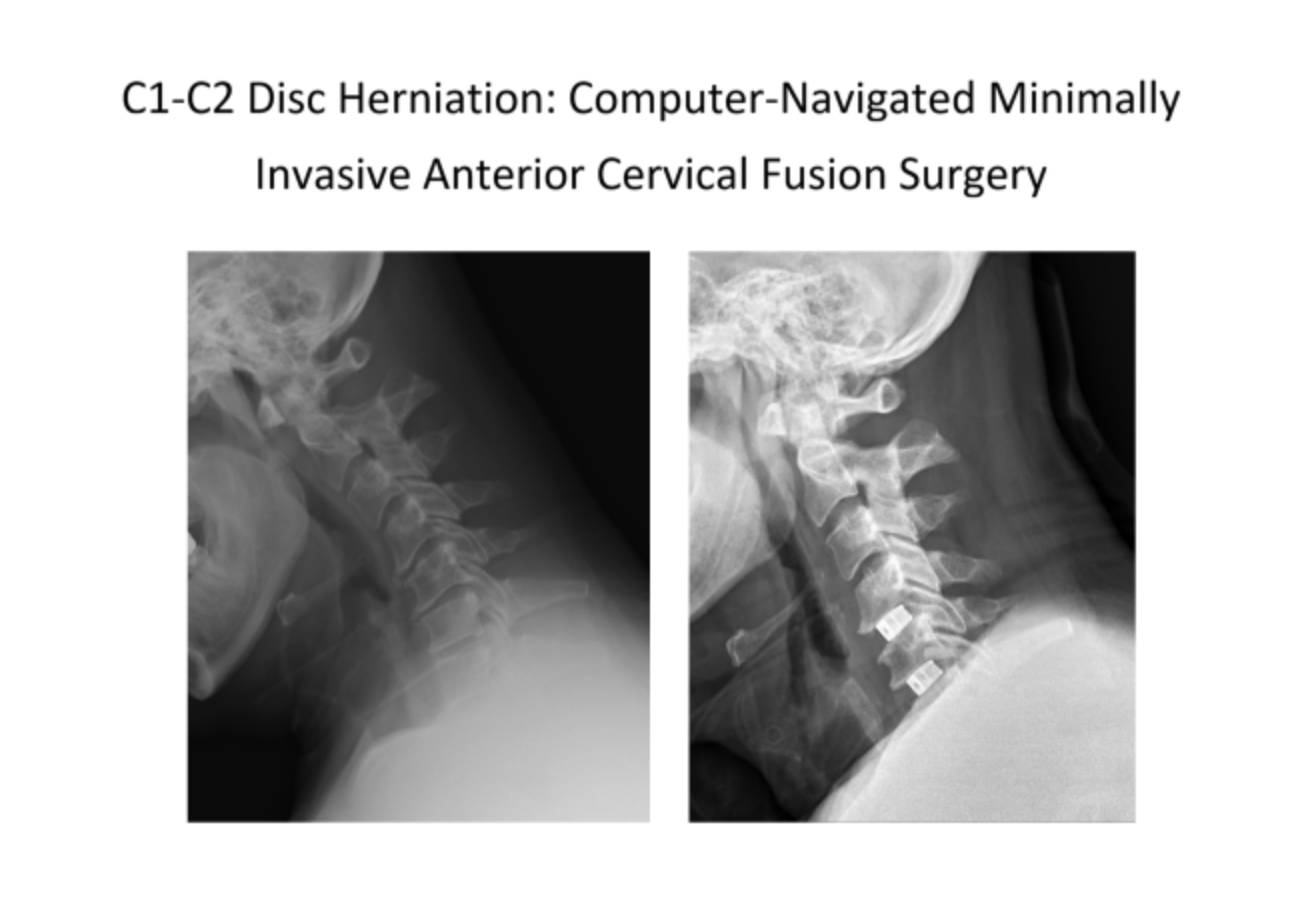
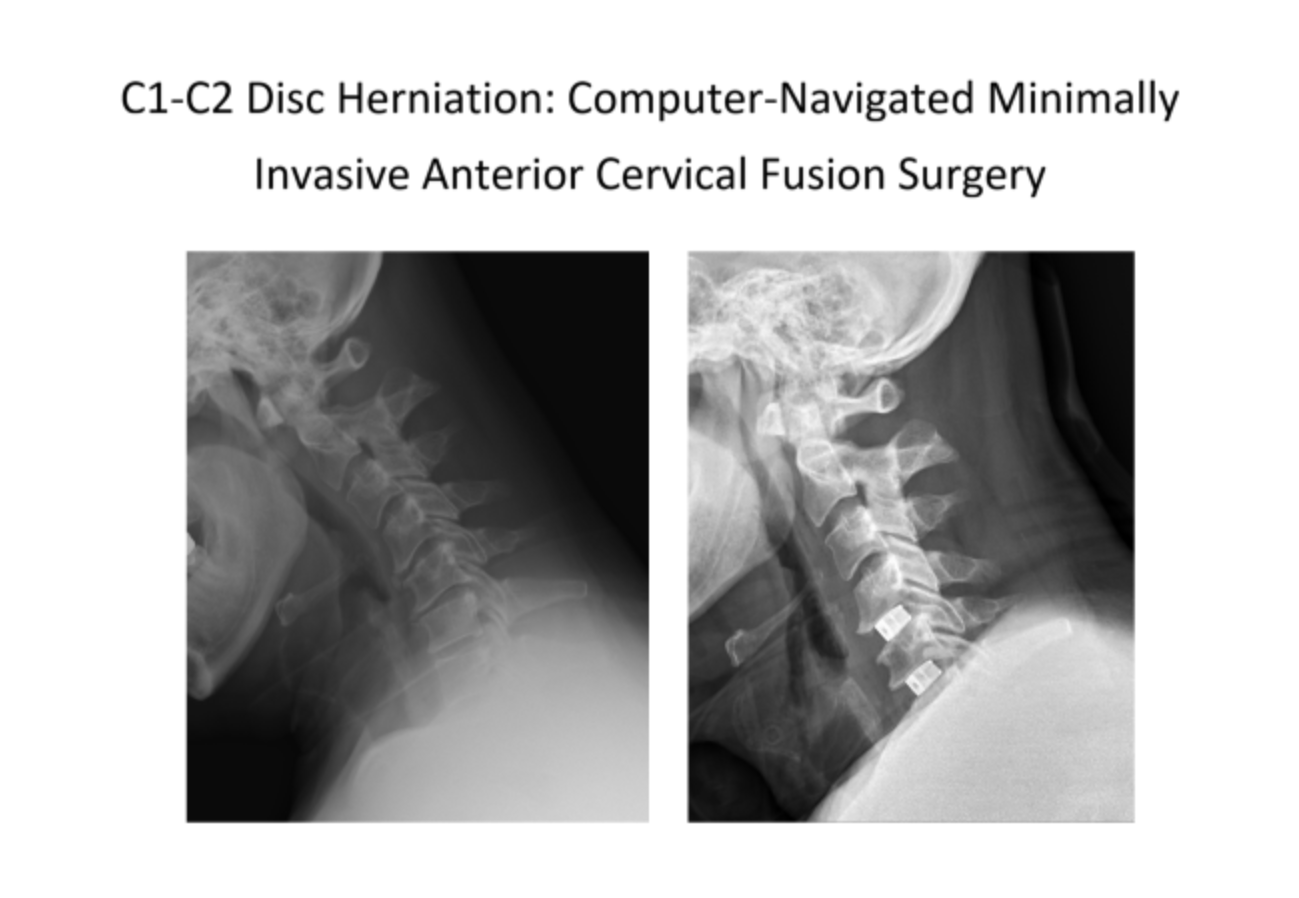
*Image caption: A case of computer-navigated minimally invasive anterior cervical discectomy and fusion. The patient was diagnosed with a C1-C2 disc herniation compressing the nerve preoperatively. The surgery involved precise implantation of an artificial disc through a minimally invasive incision, leading to rapid recovery.*
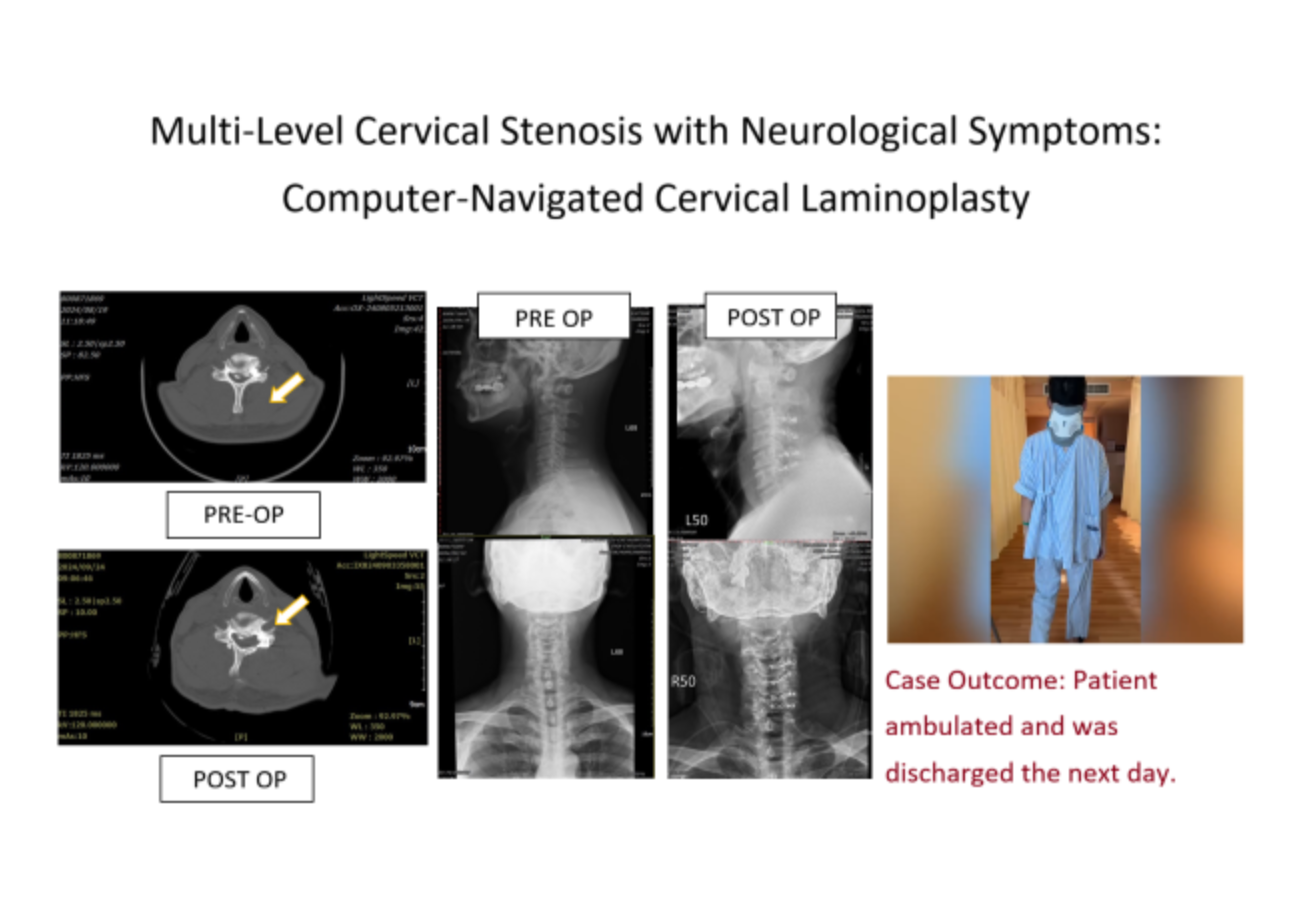
Posterior Cervical Surgery (Posterior Approach) & Laminoplasty
Posterior cervical surgery involves accessing the spinal canal through a small incision in the back of the neck. After making the incision, the muscles are carefully separated to expose the spinous processes and laminae. Decompression can be achieved via:
- Laminectomy: Complete removal of the lamina and ligamentum flavum to widen the spinal canal.
-
Laminoplasty: The lamina is preserved but hinged open like a "door" and secured with small plates, creating more space for the spinal cord.
Advantages & Risks of Posterior Cervical Surgery
Advantages
-
Ideal for Multi-Level Disease: Can address compression across several segments in one procedure.
-
Avoids Anterior Structures: Bypasses the need to navigate around the trachea, esophagus, and major blood vessels.
-
Excellent Visualization: Provides a wide view for thoroughly addressing posterior pathologies like thickened ligaments.
-
Preserves Motion (Laminoplasty): Laminoplasty maintains the bony structure and may reduce long-term adjacent segment degeneration risk.
Risks / Considerations
-
Postoperative Discomfort: The incision is larger with more muscle dissection, making postoperative neck/back pain and stiffness more common.
-
Potential for Sagittal Imbalance: If there is pre-existing loss of cervical lordosis (normal curve), posterior decompression might allow the spinal cord to shift forward.
The Ultimate in Minimally Invasive: Cervical Endoscopic Surgery
Cervical endoscopic surgery utilizes specialized endoscopic instruments, entering from the posterior or anterior side of the neck through a very small incision to perform micro-discectomy, partial laminectomy, and nerve decompression under 64x magnified, high-definition visualization.
Potential Complications of Cervical Spine Surgery
-
-
C5 Nerve Root Palsy (manifesting as upper arm weakness and paresthesia)
-
Postoperative neck stiffness and reduced range of motion
-
Postoperative spinal instability or kyphotic deformity (especially after complete laminectomy)
-
Dural tear and cerebrospinal fluid leakage
-
Relatively long recovery period, typically requiring 3–7 days of hospitalization, with a return to full activity taking several weeks to months.
The cervical spine's structure is intricate and adjacent to the neural center, making surgery a high-risk and precise endeavor. Precisely for this reason, our team regards "safety" and "precision" as non-negotiable absolute standards.
We utilize the "3D computer navigation system" to provide real-time three-dimensional guidance with an error margin of less than 0.1 cm. Performed by an experienced team of surgeons, this transforms complex anatomical structures into clear, visualizable pathways.
This rigorous "navigation-assisted standardized protocol" not only allows us to perform many traditionally large-open surgeries in a minimally invasive manner but also fundamentally and significantly reduces risks such as nerve injury. This grants high-difficulty surgeries a predictable level of safety. -
Step 1: Precise Diagnosis – The Key to Deciding the Minimally Invasive Pathway
"Minimally invasive" is not a single surgery but a portfolio of techniques tailored to the problem. The first and most critical step is an accurate diagnosis. The type of compression dictates the surgical approach:
-
Anterior (e.g., disc herniation, bone spur)
-
Posterior (e.g., ligament hypertrophy, stenosis)
-
Multi-level Complex Disease
This assessment directly determines the safest and most effective minimally invasive route.
【Our Advantage】 Navigation & Endoscopy: The "Two Pillars" of Minimally Invasive Surgery
-
3D Computer Navigation: Acts like a real-time GPS for cervical surgery. It confirms the optimal position and trajectory of implants (e.g., artificial discs, screws) intraoperatively with sub-millimeter accuracy, drastically enhancing safety—especially crucial for revision or complex cases.
-
High-Resolution Endoscopy: Provides a crystal-clear, 64x magnified view, allowing the surgeon to precisely distinguish between nerve and pathological tissue and perform delicate decompression through an extremely small incision.
Your Cervical Problem: Which Minimally Invasive Solution Applies?
The three core techniques below can be performed with greater safety under the assistance of navigation and endoscopy.
|
Your Condition & Treatment Goal
|
Recommended Technique |
Technical Core & Advantages |
| Nerve Root Compression (primarily hand numbness/pain) OR Single-Level Anterior Spinal Cord Compression |
Navigated Anterior Cervical Minimally Invasive Surgery |
• A small incision of approximately 2-3 cm is made in the front of the neck.
• Under navigation guidance, an artificial disc is precisely implanted or fusion is performed, directly removing the anterior lesion. • Advantages: Highly targeted. Can preserve mobility (artificial disc) or achieve permanent stability (fusion). |
|
Multi-Level Spinal Canal Stenosis
(primarily walking instability)
AND Good Cervical Curvature (Lordosis) |
Posterior Minimally Invasive Laminoplasty |
• Your lamina is preserved and expanded like "opening a door," permanently increasing the spinal canal space to relieve spinal cord compression.
• Advantages: Addresses multiple levels in one procedure, avoids extensive fusion, and better maintains neck mobility. |
|
Specific Posterior Lesion or Recurrent Herniation
Pursuing Ultimate Minimally Invasiveness |
Cervical Endoscopic Surgery |
• The incision is less than 1 cm, accessing the lesion through an extremely fine channel.
• Advantages: Minimal muscle disruption, significantly less postoperative pain, short hospital stay, and the fastest recovery. |
Why Complex Cervical Revision Surgery Requires an Experienced Team
The intricate anatomy makes a second cervical surgery (revision) exceptionally challenging. Our team's value lies in:
-
Accurately Diagnosing the Cause of Failure: Is it adjacent segment degeneration? Implant loosening? Or a new site of compression?
-
Safely Planning a New Pathway Under Navigation: In the presence of existing hardware and scar tissue, the navigation system is an indispensable tool for safely creating a new surgical corridor and avoiding nerve damage.
-
Integrating Techniques for the Optimal Solution: May combine anterior, posterior, or endoscopic approaches to formulate a personalized revision strategy.
Challenges and Risks
-
High Technical Threshold: Endoscopic surgery places high demands on the surgeon's skill, with a steep initial learning curve.
-
Positioning and Imaging Monitoring: Intraoperative precise positioning and navigation are required to avoid nerve injury and incomplete decompression.
-
Complications: Include nerve injury, postoperative hematoma, swallowing difficulties, C‑5 nerve palsy, neck stiffness, etc.
-
Long-term Risks: Following fusion, adjacent segment degeneration, reduced spinal mobility, or inconveniences due to activity limitations may occur.
Postoperative Care Strategy and Rehabilitation
-
Wearing a Cervical Collar: Often necessary post-surgery to maintain spinal alignment for a period of time.
-
Early Ambulation and Progressive Therapy: Early out-of-bed activity, gradual physical therapy, and spinal core muscle training are recommended.
-
Regular Imaging Follow-up: (X‑ray/MRI) to ensure good fusion status.
-
Lifestyle and Health Management: Smoking cessation, nutritional supplementation, diabetes control, etc., aid in healing and reduce the risk of pseudoarthrosis.
-
Monitoring for Long-term Changes: Adjacent segment degeneration and spinal deformation trends need to be monitored.
Frequently Asked Questions
Q: Is cervical spine surgery very risky? How do you reduce the risks?
Any surgery carries risks; the key lies in "risk management." We minimize risks through a triple-safeguard approach:
-
Intraoperative Real-Time Monitoring: We use "Intraoperative Neuromonitoring," which acts like an alarm system for nerves, providing immediate warning if signal abnormalities occur.
-
Navigation for Precision and Risk Avoidance: We rely entirely on "3D Computer Navigation," which provides millimeter-accurate pathways, perfectly avoiding critical nerves and blood vessels.
-
Standardized Team Protocol: An experienced specialist team executes standardized surgical and care protocols to ensure consistent safety. This systematic management is precisely the core reason we can safely perform high-difficulty surgeries in a minimally invasive way.
Q: Are hoarseness or swallowing difficulties after surgery permanent?
These are potential temporary conditions that may occur after anterior approach surgery, mainly due to swelling of the tissues surrounding the laryngeal nerves. For the vast majority of patients, they are temporary. As the swelling naturally subsides over a period of several weeks to months, the symptoms will significantly improve or completely resolve. Our team will provide clear postoperative care guidelines and close follow-up to assist you smoothly through the recovery period.
Q: How long of a leave from work is needed after surgery? When can I return to work?
The recovery period depends on your surgical technique and the nature of your work:
-
Hospital Stay: Approximately 1 to 3 days.
-
Office Work: Usually, a gradual return is possible 1 to 2 weeks later.
-
Manual Labor: Requires 1 to 3 months, and can only be resumed after a physician's assessment confirms joint stability and muscle strength recovery.
The goal of minimally invasive surgery is precisely to shorten this period of impact on daily life as much as possible.
Q: Under what circumstances should cervical minimally invasive surgery be considered?
Surgery should be considered for evaluation when conservative treatments (such as medication, rehabilitation) show poor effectiveness after 3 to 6 months, and imaging tests (such as MRI) show clear structural compression of neural structures accompanied by corresponding symptoms (such as hand numbness, weakness, unsteady gait). Common indications include:
-
Cervical Disc Herniation
-
Spinal Canal Stenosis (central or foraminal type)
-
Ossification of the Posterior Longitudinal Ligament
-
Severe Bone Spur Compression
-
Some cases of spinal instability due to trauma or degeneration
Q: What are "Anterior" and "Posterior" surgeries? How does the doctor choose for me?
This depends on "the location of the compression source" and "your spinal structure":
-
Anterior Surgery: Enters from the front of the neck. Primarily addresses compression from the front, such as disc herniation or vertebral body bone spurs. It can be combined with either "Artificial Disc Replacement" (preserves mobility) or "Vertebral Body Fusion" (provides permanent stability) as the situation warrants.
-
Posterior Surgery: Enters from the back of the neck. Primarily addresses multi-level spinal canal stenosis or compression from posterior structures (such as thickened ligaments). Among these, "Laminoplasty" can enlarge the spinal canal while preserving bone, making it the preferred choice for multi-level pathologies.
The physician will make a comprehensive judgment based on your imaging, symptoms, and activity needs, choosing the most direct and safest decompression path.
Q: In anterior cervical surgery, what is the difference between "Fusion" and an "Artificial Disc"?
Both are used after anterior surgery for decompression, but their long-term goals differ:
-
Spinal Fusion Surgery: Fixes adjacent vertebral bodies into a single unit, providing permanent, rigid stability. It is suitable for patients with multi-level pathologies or pre-existing spinal instability.
-
Artificial Disc Replacement: Replaces the diseased disc with a mobile implant. While relieving compression, it preserves mobility at that segment, helping to reduce the future burden on adjacent segments.
The choice between them requires comprehensive consideration of your age, occupation, mobility expectations, and overall spinal condition. We will discuss this with you in detail before surgery.
The cervical spine is the central pathway of life; surgical choices must be made with utmost care. Let a professional team clarify your doubts. Schedule an evaluation with the [Dr. Chien-Chun Chang Minimally Invasive Spine & Joint Team]. Through detailed imaging examinations and diagnosis, leveraging the advantages of navigated minimally invasive technology, we will work with you to develop a safe, effective, and short-recovery personalized cervical spine treatment plan.






