The Complete Guide to Spine Revision Surgery: When a "Second Surgery" Becomes Necessary, How to Control the Risks?
"Doctor, I've already had surgery, so why is my back still in so much pain?" "Another doctor said my spine is full of scar tissue, and a second surgery would be too risky..."
These are situations where secondary spine surgery may be necessary. "Spinal revision surgery" is considered one of the most challenging fields in spine surgery, primarily addressing issues such as postoperative recurrence, adjacent segment degeneration, or hardware loosening.
【Article Summary】 This article is authored by Dr. Chien-Chun Chang's team, providing an in-depth analysis of why spinal revision surgery requires more precise strategies and how we help patients regain their quality of life despite complex conditions.
-
Challenges of Revision Surgery: Secondary spine surgery often faces nerve adhesions, scar tissue, and bone defects, which increase surgical risk.
-
Precision Technology: Dr. Chien-Chun Chang's team employs O-arm 3D digital computer navigation (intraoperative GPS) and intraoperative neuromonitoring to control precision within 0.1 cm, avoiding dangerous areas.
-
Innovative Approach: Using the OLIF (Oblique Lumbar Interbody Fusion) lateral approach to bypass old back scar tissue and reconstruct from a new pathway, significantly reducing bleeding and nerve injury rates.
-
Key to Success: Combining rigorous imaging diagnostics with minimally invasive techniques to help patients who have experienced previous surgical failure regain their quality of life.
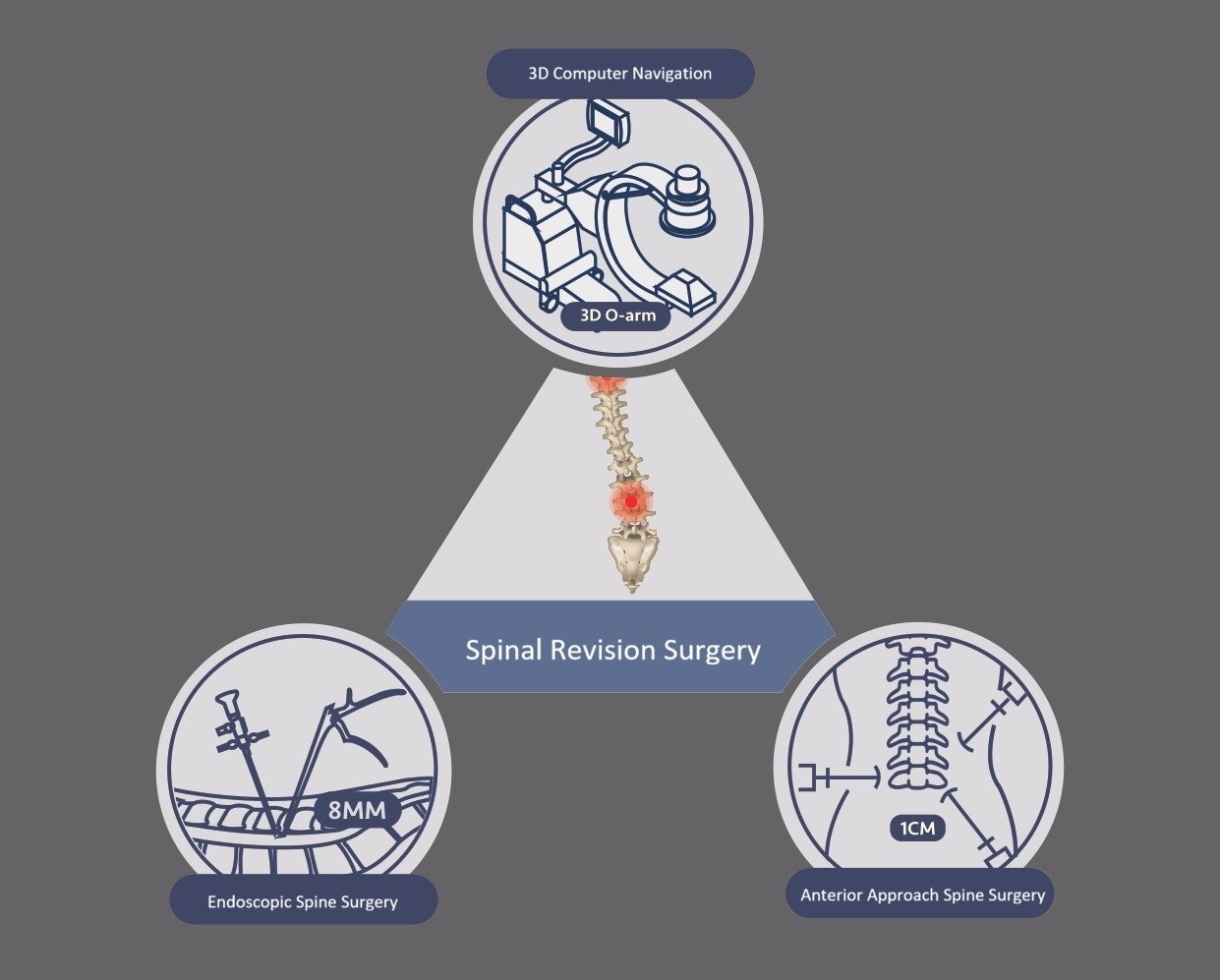
Why is "Spinal Revision Surgery" Needed?
Spinal revision surgery refers to a second course of treatment performed after a patient has previously undergone spine surgery, due to various reasons such as symptom recurrence, worsening of the condition, or the emergence of new complications.
1. Common Reasons for Revision
-
Failed Back Surgery Syndrome:
Persistent pain after surgery, which may originate from incomplete decompression or nerve adhesions.
-
Adjacent Segment Degeneration:
While the originally fused segment is stable, the adjacent spinal segments above and below degenerate at an accelerated rate due to increased stress.
-
Hardware Loosening or Fracture:
Internal fixation devices (screws, rods) may shift or break due to osteoporosis or incomplete bone fusion.
-
Pseudoarthrosis (Non-union):
The bones fail to fuse together as expected after surgery, leading to chronic instability and pain.
-
Postoperative Infection or Hematoma:
Acute complications that require immediate intervention.
| Reasons for Revision |
Primary Etiological Diagnosis |
Clinical Presentation | Treatment Strategy |
|
Failed Back Surgery Syndrome |
Incomplete Decompression / Nerve Adhesion
|
Persistent postoperative aching, numbness
|
Navigated precise decompression and neurolysis (nerve release) |
|
Adjacent Segment Degeneration |
Adjacent Segment Disease (ASD) | Spinal stenosis or spondylolisthesis in segments above/below the original surgery site |
Decompression surgery with extension of the fixation construct to adjacent levels
|
| Structural Failure | Screw Loosening, Fracture, Migration |
Localized severe back pain, poor weight-bearing sensation
|
Removal of old hardware and re-fixation using a new, stable trajectory
|
| Biomechanical Failure | Pseudoarthrosis (Non-union) | Chronic instability pain due to postoperative non-fusion of bone |
Re-debridement, bone grafting, and enhanced fusion support
|
| Surgical Complication | Infection, Hematoma, Dural Tear | Sudden postoperative redness, swelling, heat, pain, worsening limb weakness |
Acute debridement and drainage, dural repair surgery
|
2. Secondary Correction After Scoliosis Surgery
For adolescent or adult scoliosis surgery, if the initial surgical correction is insufficient, or if spinal imbalance develops with age, revision surgery is required to readjust the spinal curvature.
The Difficulties of Revision Surgery: Challenges from the Surgeon's Perspective
Why do many physicians approach revision surgery with caution? The reason lies in the altered physiological environment within the spine:
-
Scar Tissue
Scar tissue from the previous surgery encases the nerve roots, obscuring the normal anatomy and increasing the risk of accidental nerve injury.
-
Bone Defect
The void left in the bone after removing old screws makes re-fixation difficult.
-
Structural Distortion
Severe scoliosis revision often involves complex 3D deformities. Traditional X-rays are insufficient for adequate surgical assessment and guidance.
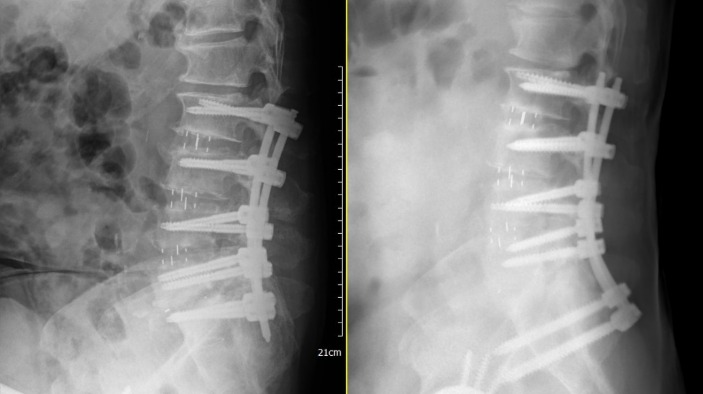
Surgical Techniques and Principles for Spinal Revision
When facing complex revisions, we no longer rely on traditional methods involving "large incisions and forceful dissection." Instead, we perform secondary revision through 3D digital computer navigation combined with multiple minimally invasive approaches.
1. Advantages of 3D Digital Computer Navigation (O-arm)
In revision surgery, the navigation system acts as the surgeon's "GPS" and "X-ray vision," providing the following benefits for a more precise and safer procedure:
2. Lateral Lumbar Revision Surgery (OLIF / Lateral Approach)
| Comparison Metrics | Traditional Open Revision | Computer-assisted Navigated Minimally Invasive (OLIF) |
| Surgical Approach | Access via the old incision (significant scar tissue/adhesions) | New lateral approach (avoids adhesions) |
| Blood Loss | Higher, often requires blood transfusion | Significantly reduced, risk manageable |
| Risk of Nerve Injury | Higher (due to obscured anatomy) | Low (dual protection from nerve monitoring & navigation) |
| Postoperative Recovery | 3-6 months | 1-3 months |
3. New Minimally Invasive Spinal Endoscopy (with 3D Computer Navigation)
Utilizes high-magnification microscopy and ultrasonic bone scalpels to minimally invasively address nerve adhesions, reducing intraoperative blood loss and lowering the risk of nerve damage.
Evaluating Indications for Spinal Revision Surgery: Are You a Suitable Candidate for Another Operation?
Not all postoperative pain is suitable for surgical intervention. Dr. Chien-Chun Chang's team conducts a rigorous "Three-Step Revision Assessment":
1. Imaging Diagnosis
Utilizes dynamic X-rays (flexion/extension), high-resolution MRI (spinal magnetic resonance imaging), and CT (computed tomography) scans to determine the presence of structural instability or compression.
2.Neurophysiological Diagnosis
Performs electromyography (EMG) or nerve conduction studies to confirm the origin of the pain.
3.Pain Source Identification
Sometimes pain originates from pelvic imbalance or myofascial issues. In such cases, the effectiveness of rehabilitation therapy may be superior to surgery.
Risks of Revision Surgery: Transforming "Variables" into "Controlled Factors"
Facing a second surgery, what patients fear most is the "risk." At Dr. Chien-Chun Chang's team, we employ a standardized precision protocol to significantly reduce the risks associated with complex revision surgery.
1. Prevention of Nerve Injury: Dual Safeguards
-
Intraoperative Neuromonitoring (IONM)
During the procedure, monitoring equipment continuously tracks nerve conduction signals. If the surgeon approaches a nerve's boundary or if a nerve is stretched, the system provides immediate auditory and visual alerts. This is a monitoring function we heavily rely on in revision areas dense with scar tissue.
-
Real-Time Navigation Positioning
Coupled with 3D digital navigation, we can accurately predict the path of nerve roots deep within the bone, avoiding nerve damage during surgery.
2. Reducing Blood Loss and Infection Control
-
Minimally Invasive Approach: Revision surgery often requires a longer operative time. Employing the lateral (OLIF) approach, which avoids extensive dissection of the back muscles, can significantly reduce intraoperative blood loss, thereby lowering the risk of infection.
-
Ultrasonic Bone Scalpel: For patients requiring the removal of old bone spurs or bone cement, the ultrasonic scalpel allows for precise cutting of hard tissue without damaging surrounding soft tissues (nerves and blood vessels).
3. Enhancing Bone Fusion Rates
or revisions addressing "pseudoarthrosis" or "hardware loosening," we often combine bone morphogenetic protein (BMP) or autologous bone graft. During surgery, we utilize the digital navigation system to ensure the interbody cage is placed along the path of maximum mechanical support, guaranteeing that the secondary surgery achieves true bone fusion.
Spinal Revision Surgery FAQ
Here are authoritative answers from Dr. Chien-Chun Chang to the core questions most concerning to patients considering a second surgery:
Q:If the first surgery was not successful, will the second one be more difficult and dangerous?
Dr. Chang's Perspective: It is technically more challenging, but the risks are controllable. The challenge of revision surgery lies in the disrupted anatomy and dense scar tissue, which do pose higher risks for traditional methods. However, with the introduction of modern 3D digital computer navigation (O-arm), we now have an intraoperative "navigation map" that allows us to precisely avoid nerves and accurately place implants. As long as the surgeon is experienced and the equipment is advanced, the success rate and safety of revision surgery have been significantly improved.
Q: What is the recovery period for spinal revision surgery?
Dr. Chang's Perspective: The recovery period depends on the surgical approach. If navigated minimally invasive revision can be performed, most patients can walk with a brace within 2-3 days after surgery, with a hospital stay of approximately 5-7 days. Because minimally invasive surgery causes less muscle damage, postoperative pain in the early stages is significantly milder compared to traditional open revision. Most daily activities can be resumed around 3 months postoperatively.
Q: Why is my doctor suggesting a "lateral" approach for my revision surgery?
Dr. Chang's Perspective: This typically refers to OLIF (Oblique Lumbar Interbody Fusion). In revision cases, the back often has severe adhesions (scar tissue) from the previous surgery. The "lateral" approach provides a completely new pathway that entirely avoids the old scar tissue and nerves. It offers not only strong corrective force and the ability to place a larger interbody cage but also enhanced safety. This is currently a mainstream international trend for managing revision surgery.
Q: Does revision surgery always require removing the old screws?
Dr. Chang's Perspective: Not necessarily. The decision is based on whether the old screws are loose, infected, or obstruct the new corrective path. If the old screws are still stable and their position is not a hindrance, we may sometimes leave them in place and reinforce other segments. Using the navigation system, we can precisely assess the spatial relationship between the old and new screws to formulate the most streamlined and effective implant strategy.
Postoperative Recovery and Life Rebuilding: The Path to Renewal After Revision
The success of the revision surgery is just the beginning. Postoperative care and rehabilitation are the keys to maintaining long-term results.
-
Phased Activity Restrictions
-
Within 1 month after surgery, strictly avoid bending, lifting heavy objects, or prolonged sitting.
-
For the long-term health of your spine, it is also recommended to continuously avoid these postures or actions that place stress on the spine, cultivating good habits to prevent recurrence.
-
Core Muscle Training
-
Under the guidance of a physician and physical therapist, perform "isometric contraction" exercises to strengthen spinal stability.
-
Osteoporosis Treatment
-
Many revisions are due to hardware loosening caused by insufficient bone quality. Therefore, postoperative osteoporosis medication (such as calcium, vitamin D, or specific bone-building drugs) must be implemented concurrently.
Conclusion: Don't Let One Setback Limit Your Desire for Mobility
While "spinal revision surgery" may sound daunting, in today's era of precision medicine, it is no longer synonymous with high risk. Dr. Chien-Chun Chang's team is dedicated to utilizing 3D digital computer navigation systems and minimally invasive approaches to carve out a safe path for patients amidst dense scar tissue and imbalanced structures. If you are suffering from persistent postoperative pain or have been told a second surgery is necessary, remember this: Leave the complex anatomy to navigation technology, and entrust your anxiety to our professional team for care.
This article is for educational purposes only. Please be sure to consult a qualified physician for specific medical advice.






