The Complete Guide to Scoliosis Surgery: From the Golden Window of Treatment to Minimally Invasive Techniques — A Surgeon’s Explanation of Key Factors for Safe Correction
【Article Summary】 This article is authored by Dr. Chien-Chun Chang's medical team, providing an in-depth analysis of the core technologies in modern scoliosis surgery.
Surgical Criterion: Surgery should be considered for adolescents with a Cobb angle exceeding 40°-45°, or for adults when the deformity is accompanied by neurological compression.
Optimal Timing: For adolescents, optimal correction is achieved before skeletal maturity (Risser Sign grades 3-4). For adults, intervention is recommended before functional decompensation occurs.
Precision Technology: The introduction of the O-arm computer navigation system reduces implant placement error to under 0.1 cm, significantly enhancing surgical safety.
Advantages of Minimally Invasive Techniques: Modern minimally invasive approaches minimize incision size and reduce blood loss, enabling most patients to ambulate the day after surgery.
Risk Management: By integrating intraoperative neuromonitoring, the risk of complications is minimized. The overarching goal is to restore spinal biomechanical balance and improve quality of life.
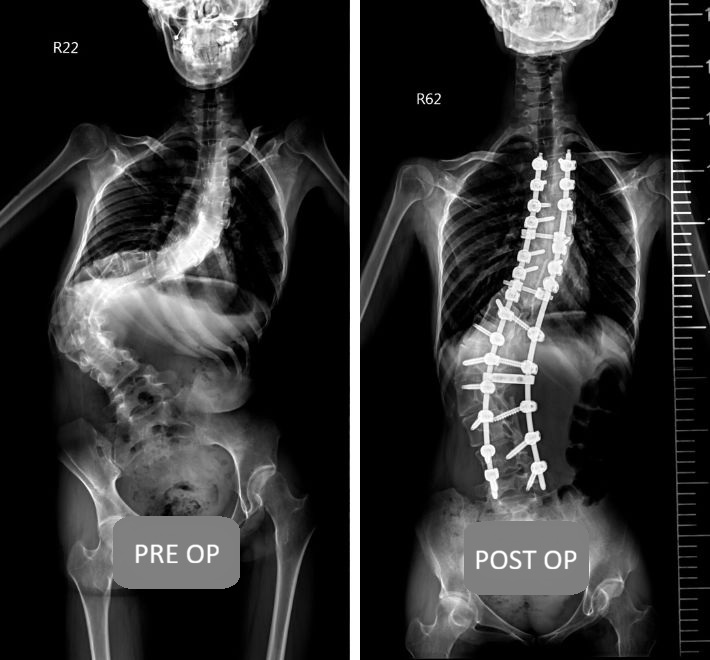
Regarding spinal surgery, patients' most common questions typically revolve around "safety" and "necessity," often asking: "Doctor, is surgery absolutely necessary for scoliosis?" or "Could the surgery damage nerves and lead to paralysis?"
With modern medicine entering the era of "precision medicine," scoliosis surgery has evolved from traditional large-incision, experience-dependent procedures to the integration of 3D digital computer navigation (O-arm) and diverse minimally invasive techniques. This advancement not only significantly reduces the size of surgical incisions but also elevates precision to the millimeter level.
This article is authored by Dr. Chien-Chun Chang's Minimally Invasive Spine & Joint Team, providing an in-depth analysis of the core principles and recovery process of contemporary scoliosis surgery.
When Should "Scoliosis Surgery" Be Considered?
Not all patients with scoliosis require surgery. Physicians conduct a comprehensive evaluation based on the Cobb's Angle (curve magnitude), skeletal maturity (Risser Sign), and clinical symptoms.
Related Article: Scoliosis: A Comprehensive Guide — Types, Screening & Minimally Invasive Correction
1. Surgical Indications
According to guidelines from the Scoliosis Research Society (SRS), surgical intervention is typically recommended for evaluation under the following conditions:
-
Rapid Curve Progression: In adolescents, a Cobb angle exceeding 40°-45° that continues to progress at a rate of more than 5° per year.
-
Physiological Impairment: Severe curvature compresses the thoracic cavity, leading to decreased cardiopulmonary function or restrictive lung disease.
-
Neurological Compression & Pain: Adult scoliosis accompanied by severe degeneration, resulting in symptoms such as neurogenic claudication, sciatica, or spinal stenosis.
-
Severe Cosmetic Deformity: Significant physical deformities like uneven shoulders, a rib hump ("razor back"), or thoracic torsion that cause physical discomfort or psycho-social distress for the patient.
2. The "Golden Window" for Undergoing Scoliosis Surgery
The timing of surgery directly impacts the correction rate and recovery speed. Clinically, there are two key windows:
-
The Adolescent Golden Window (Before Skeletal Maturity):
The optimal time for intervention is typically at Risser Sign 3-4 (when the pelvic growth plates are nearly fused), if the Cobb angle has already reached the surgical threshold. At this stage, the spine retains a degree of flexibility. This allows surgeons to achieve greater angular correction with less corrective force, and post-operative bone fusion occurs very rapidly. -
The Adult Critical Window (Before Symptom Decompensation):
For adult patients, the surgical timing is determined not by age, but by intervening before "decompensation" occurs. Surgery should be considered when scoliosis leads to significant trunk imbalance, worsening pain, or a reduced walking distance (claudication). The goal is to prevent long-term spinal imbalance from accelerating degeneration in adjacent spinal segments.
Comparison Item |
Adolescent Idiopathic Scoliosis (AIS) |
Adult Spinal Deformity (ASD) |
|
Primary Goal |
Correct curvature, prevent future progression |
Relieve nerve compression, restore physiological balance |
|
Optimal Timing |
Late skeletal development (Risser 3-4) |
Early stage of worsening pain or functional limitation |
|
Main Patient Concern |
Cosmetic deformity, cardiopulmonary compromise |
Sciatica, inability to stand/walk for prolonged periods |
Technological Revolution: Digital Computer Navigation Enhances "Safety"
Traditional spine surgery relied on the surgeon's experience and intraoperative 2D imaging, akin to navigating the human body with a flat map. When addressing complex conditions like scoliosis, 2D imaging often presented blind spots. This paradigm shifted with the advent of O-arm digital navigation systems, which have significantly elevated surgical precision and safety.
1. Intraoperative GPS: The O-arm Real-Time Digital Navigation System
The intraoperative real-time 3D digital computer navigation (O-arm) system we have introduced is hailed as the "GPS of the operating room." Its value for scoliosis surgery lies in the following:
-
Real-Time Scanning: Performs 3D scans during surgery, with the screen displaying the real-time relative positions of spinal structures, nerves, and implants.
-
High Precision: Controls implant placement error to < 1 mm, a critical factor in the distorted bony anatomy of scoliosis.
-
Dynamic Screw Placement: Enables surgeons to accurately place multiple pedicle screws dynamically, significantly improving the correction rate while further minimizing neurological risk.
2. Reduced Radiation Exposure
Compared to traditional methods that require repeated intraoperative X‑ray imaging, the O‑arm digital navigation system significantly reduces the radiation dose received by both the medical team and the patient during the surgical procedure.
If you are facing the choice of scoliosis correction treatment, evaluating the final outcome is just one part of the decision. The safety during the procedure and the quality of recovery afterward are equally, if not more, crucial.
Dr. Chien-Chun Chang's team is dedicated to advancing the minimally invasive transformation of complex spinal surgeries. Our foundation of excellence is built on the integration of "precision," "safety," and "extensive experience." Therefore, we employ the O-arm integrated 3D computer navigation system, which provides real-time visualization of vertebral anatomy and implant positioning during surgery. This allows us to control placement error within an extremely minute range and to dynamically and accurately place each pedicle screw, significantly enhancing procedural safety.
However, the most advanced technology requires operation by experienced surgeons. Dr. Chang's team has accumulated substantial experience in navigated minimally invasive scoliosis surgery, mastering the art of transforming real-time 3D navigation data into a personalized correction strategy best suited to an individual's unique spinal structure. Our commitment to quality is also validated by our SNQ (Symbol of National Quality) certification.
If you are seeking a minimally invasive scoliosis solution that balances a high correction rate with high safety, you are welcome to bring your imaging studies and all your questions for an in-depth consultation with Dr. Chang's team. Let us conduct a thorough evaluation for you and jointly formulate a truly patient-centered, reassuring, and precise treatment plan.
Mainstream Surgical Techniques: From Traditional Instrumentation to Modern Minimally Invasive
There is no single "standard answer" for scoliosis surgical techniques; instead, the approach is "tailor-made" based on the patient's age, curve complexity, and bone quality.
1. Traditional Technique: Posterior Spinal Instrumentation and Fusion (The Gold Standard)
While modern minimally invasive techniques are prevalent, traditional open surgery remains the ideal approach for treating extremely severe deformities or multi-level complex curves.
-
Principle: A midline incision is made on the back, muscles are retracted to provide a clear field of view, screws are implanted, corrective osteotomies are performed, and bone graft is added to achieve fusion.
-
Advantages: Provides the strongest corrective force and the most direct visual field, making it suitable for complex cases with curves greater than 70°.
-
Disadvantages: Larger incision (typically 15-30 cm), greater blood loss, and more significant muscle disruption.
2. Modern Minimally Invasive Techniques: Balancing Precision and Rapid Recovery
With the support of 3D digital computer navigation, minimally invasive surgery has become the preferred choice for many cases of adult degenerative scoliosis and moderate adolescent scoliosis.
-
Oblique Lumbar Interbody Fusion (OLIF) / Lateral Lumbar Interbody Fusion (LLIF):
The spine is accessed from the side of the abdomen, avoiding the posterior nerve plexus. This technique allows for the implantation of interbody cages that are up to three times larger than those used in traditional surgery, utilizing the "lever principle" to restore disc height. It offers excellent correction while preserving the back muscles. -
O-arm 3D Computer-Navigated Minimally Invasive Correction:
Pedicle screws are placed with precision through small incisions under the guidance of the O-arm navigation system. Studies show this technique can reduce blood loss by approximately 50-70%, allowing patients to ambulate within 1-2 days after surgery. -
Endoscopic Surgery:
For localized scoliosis accompanied by "herniated discs" or "single-level stenosis", this approach provides the most minimally invasive decompression solution, with an incision of only about 1 cm.
Surgical Technique Categories |
Applicable Candidates |
Primary Advantages |
Potential Challenges |
| Traditional Posterior Fusion |
Extremely severe scoliosis, complex revision cases |
Strongest corrective force, clearest visual field |
Larger incision, longer recovery period |
| Minimally Invasive Navigation / OLIF |
Adult degenerative scoliosis, |
Minimal blood loss, rapid ambulation, low post-op pain | Extremely high demands on surgeon's skill and equipment |
| Growth-Guided Surgery |
Children under 10 years old, still developing |
Balances correction with spinal growth and development |
Requires long-term follow-up and length adjustments
|
| Endoscopic Surgery | Single-level stenosis accompanied by mild scoliosis | Extremely small incision, potential for local anesthesia | Cannot address large-scale deformities |
3. For Growing Children: Growth-Guided Scoliosis Correction Surgery
For children under the age of 10 with early-onset scoliosis whose skeletons have not yet matured, the goal is "to control the curvature while allowing for spinal growth."
-
Extendable Connecting Rods: Following the initial surgery, regular follow-up is required. Once the patient has passed through the growth period, permanent fixation can be achieved through a final surgical procedure.
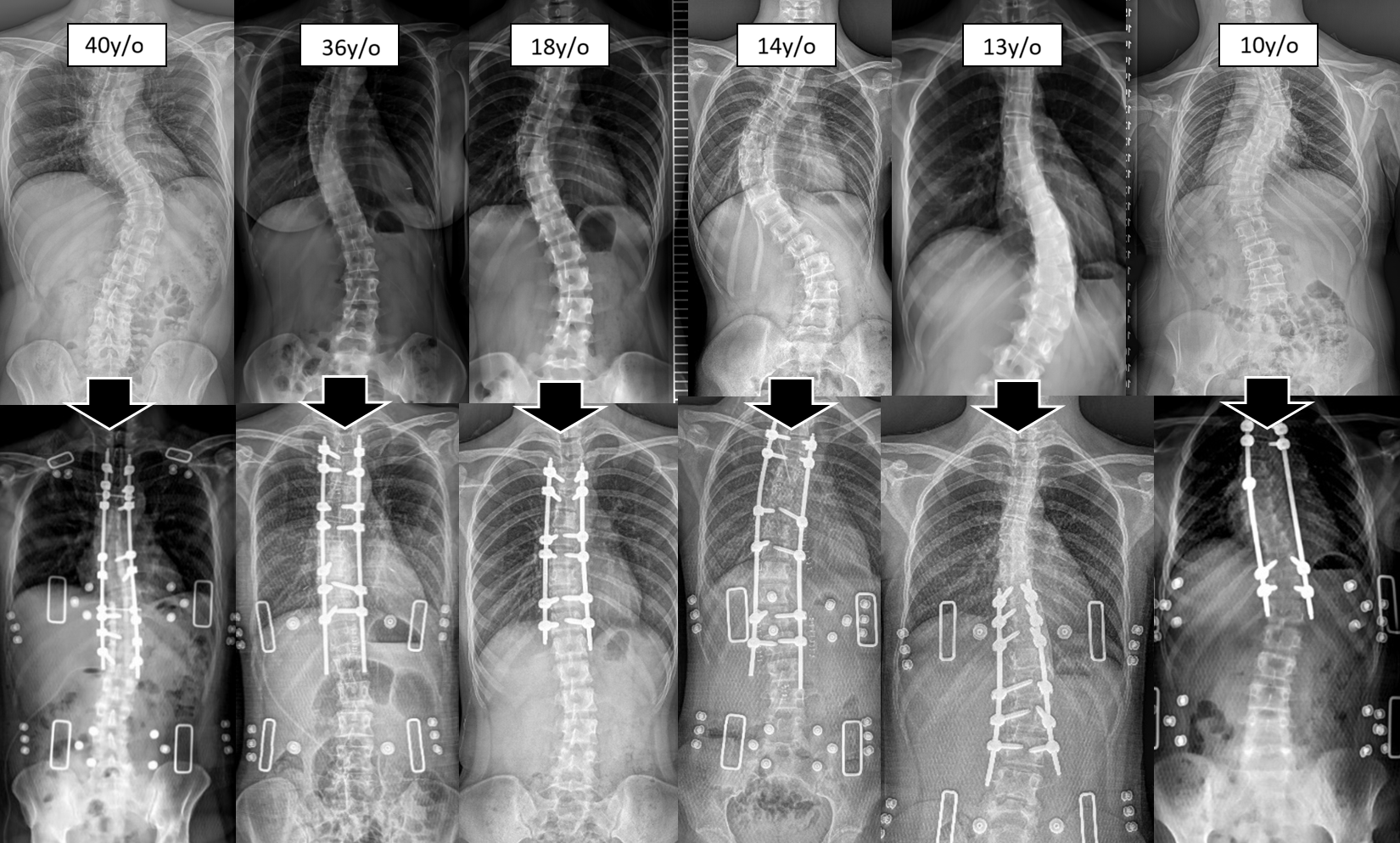
Facing scoliosis of different ages and curve types, Dr. Chien-Chun Chang's team always upholds professionalism and patience. With our extensive accumulated experience in minimally invasive surgery, we tailor safe and effective correction strategies for each patient, accompanying you steadily toward health.
4. Minimally Invasive Approach to Complex Spinal "Revision Surgery"
For patients who have undergone previous scoliosis surgery but experienced suboptimal outcomes, hardware loosening, or adjacent segment degeneration, traditional revision surgery often necessitates an extremely large incision.
The Hallmark of Dr. Chang's Team in Revision Surgery: Leveraging extensive clinical experience in diagnostic interpretation, our team utilizes 3D digital computer navigation to accurately navigate through dense scar tissue and avoid nerves. This allows us to perform "minimally invasive" revision surgery, transforming what was traditionally a highly invasive procedure.
What Patients Care About Most: Postoperative Recovery and Risk Management
1. Will I become taller after surgery? Will I lose mobility?
-
Increase in Height: Following scoliosis correction, as the curved spine is straightened, patients typically experience a feeling of having "grown" by several centimeters.
-
Considerations for Mobility: The surgical goal is to "preserve mobility where it should move and achieve stability where it should be stable." For adolescent patients, we strive to preserve as many motion segments as possible. For adult patients, the primary goals are to resolve pain and restore walking function. Typically, mobility in the thoracic spine segments can be largely preserved.
2. Recovery Period and Pain Management
-
Early Ambulation: Most patients undergoing minimally invasive scoliosis surgery can get out of bed and walk with a brace within 2-4 days postoperatively.
-
Hospital Stay: Navigated minimally invasive surgery typically requires a hospital stay of only approximately 5-7 days.
-
Gradual Rehabilitation: The focus is on "gradual, progressive activity" rather than "prolonged bed rest" to avoid complications associated with immobility.
3. Risk Prevention: Standardized Protocols
While any surgery carries inherent risks (such as bleeding, infection, or nerve injury), Dr. Chang's team, recognized as "Taiwan's First International Computer Navigation Demonstration Center," has established rigorous standardized protocols:
-
Preoperative: Meticulous planning based on MRI/CT scans, comprehensive anesthesia assessment, and pre-surgical patient education on physical therapy.
-
Intraoperative: Utilization of the O-arm digital computer navigation system along with real-time intraoperative neuromonitoring to minimize risks to the greatest extent possible.
Scoliosis Surgery FAQ (Frequently Asked Questions)
The following are answers to the five most common core questions about scoliosis surgery, provided by Dr. Chien-Chun Chang:
Q: What is the success rate of scoliosis surgery? Is there a risk of paralysis?
Dr. Chang's Perspective: With modern precision medicine, the safety of scoliosis surgery has been greatly enhanced. According to clinical data, when combining 3D digital computer navigation with intraoperative neuromonitoring, the risk of paralysis due to nerve injury has been reduced to less than 1%. Any abnormality is detected and alerted immediately during the surgery.
Q: How should I choose between minimally invasive surgery and traditional open surgery?
Dr. Chang's Perspective: The selection criterion is based on "minimizing tissue damage while effectively solving the problem." Traditional surgery involves a large incision and extensive muscle dissection, making it suitable for extremely severe, multi-level complex deformities with very poor bone quality. In contrast, minimally invasive surgery (such as OLIF or MISTLIF) utilizes small incisions and navigated screw placement, which can significantly reduce blood loss (by approximately 50-70%) and accelerate the time to post-operative ambulation. For patients with a weaker constitution, the elderly, or those wishing to shorten their rehabilitation period, the combination of minimally invasive and navigated techniques is the preferred choice.
Q: What is the approximate cost of scoliosis surgery? Is it covered by National Health Insurance (NHI)?
Dr. Chang's Perspective: The basic costs of scoliosis surgery (such as hospitalization and standard screws/rods) are typically covered by Taiwan's National Health Insurance (NHI). However, special high-grade medical implants and auxiliary technologies require out-of-pocket payment. These may include:
-
High-Grade Titanium Alloy Implants/Cages: Offer superior biomechanical strength, beneficial for long-term fusion.
-
3D Computer Navigation System (O-arm) Usage Fee: Ensures surgical precision.
-
Ultrasonic Bone Scalpel: Reduces blood loss and bone tissue trauma.
The total cost typically ranges from several hundred thousand New Taiwan Dollars, depending on the number of spinal segments involved and the specific surgical technique used. We strongly recommend discussing **insurance reimbursement and payment options in detail with your medical team before surgery.
Q: Can I return to sports after surgery? Do the internal implants need to be removed?
Dr. Chang's Perspective: The goal after surgery is to "return to life." Once bone fusion is stable, typically 3-6 months post-operatively, most patients can resume low-to-moderate impact activities such as swimming, brisk walking, and cycling. After about one year, depending on recovery, participation in most sports is possible.
Regarding the implants, modern medical devices are made from high-biocompatibility titanium alloy. Unless an extremely rare event like infection or loosening occurs, the implants are designed to remain in place for life and do not need to be removed. They also will not trigger airport security alarms.
Q: Is scoliosis surgery effective for adults?
Dr. Chang's Perspective: Adult scoliosis often coexists with degenerative lumbar stenosis, making the surgical goals fundamentally different from those for adolescents. The focus of adult surgery is "relieving nerve compression" and "restoring spinal balance."
Through minimally invasive techniques like the Oblique Lumbar Interbody Fusion (OLIF), we can effectively correct the imbalance caused by degeneration. This leads to significant improvement in symptoms that severely impact quality of life, such as inability to stand for long periods due to pain and walking difficulties (neurogenic claudication).
Dr. Chien-Chun Chang's Team: A Core Demonstration Center for Minimally Invasive Spine Surgery in Taiwan
When choosing a surgical team, it's crucial to look beyond just technique and evaluate the "system." The Minimally Invasive Spine & Joint Center led by Director Chien-Chun Chang possesses the following three major advantages:
1. Internationally Recognized Navigation Demonstration Center
We are Taiwan's first internationally certified computer navigation demonstration center. This signifies that our standardized protocols are not only applied in clinical practice but also serve as a model for other surgeons to learn from.
2. SNQ-Certified Standardized Protocol for Complex Spine Surgery
Dr. Chien-Chun Chang's team has been awarded the prestigious SNQ National Quality Symbol certification. This recognition confirms that our techniques and protocols for "applying computer navigation to complex spinal surgeries" meet national standards for safety and quality.
We possess not only top-tier equipment but, more importantly, have established a "standardized surgical protocol." This protocol ensures that every complex spinal procedure, from preoperative planning and intraoperative navigation to postoperative care, is executed with precision and consistency, significantly enhancing surgical safety and outcomes.
3. "Patient-Centered" Precision Decision-Making
We understand that every patient's spinal curve is unique. Through preoperative 3D CT simulation, we create a customized surgical plan for each individual. We explain "why this specific procedure is suitable for you," moving away from a one-size-fits-all approach.
Conclusion: Courage Stems from Trust in Technology and Expertise
Modern scoliosis surgery is no longer the daunting, high-risk endeavor it once was. Enhanced by 3D digital computer navigation and minimally invasive techniques, we can now minimize risks and maximize benefits. If you or a loved one is suffering from scoliosis, we recommend seeking evaluation from a specialist with extensive experience in navigated minimally invasive surgery.
This article is for educational purposes only. For specific medical advice, please be sure to consult with a qualified physician.






